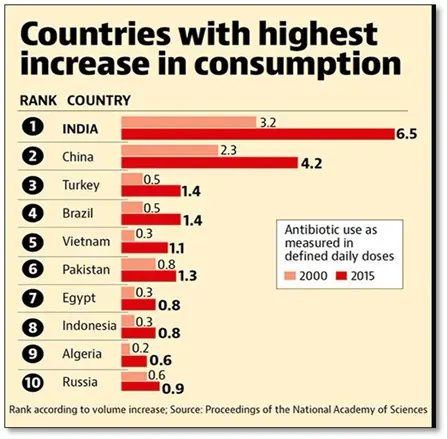
Did you know that India is called the “Antibiotic Capital of the World”? This is because India is not only the largest producer of antibiotics globally but also ranks as the largest consumer by absolute volume. The total private-sector antibiotic consumption increased by 12.0% between 2011 and 2016, from 4749 to 5358 million defined daily doses (DDDs, and then decreased to 5071 million in 2019, registering a net increase of 6.8% between 2011 and 2019. This widespread use contributes to the growing concern over antimicrobial resistance (AMR), particularly antibiotic-resistant bacteria.
In this article we talk about potential solutions for combating AMR in wastewater. We will not only investigate the advanced treatment technologies that can effectively address the rise but also emphasize the critical need for robust policies. Further, we will also explore the Drug and Cosmetics Act of 1940 and the recent framework, National Action Plan on Antimicrobial Resistance.
By integrating technological innovation with policy-driven action, we can better confront the challenges posed by antimicrobial resistance (AMR), ultimately safeguarding public health and protecting our environment.
Will advanced treatment technologies help?
Conventional wastewater treatment methods are limited in effectively removing antibiotics and antibiotic-resistant bacteria. Traditional processes like primary sedimentation and biological treatment focus on reducing organic and nutrient loads, but they often fail to adequately target pharmaceutical residues and ARGs. This gap in treatment creates opportunities for antibiotic-resistant bacteria to proliferate, turning wastewater treatment plants into potential “hotspots” for resistance development and spread. As a result, there is a pressing need for advanced treatment technologies to mitigate these risks.
Challenges in implementing advanced treatments:
Despite their promise, advanced treatment technologies face significant implementation hurdles:
- High Operational Costs: Advanced systems often require substantial investments in equipment, maintenance, and energy, making them less accessible for resource-limited facilities.
- Complexity of Operations: Advanced technologies demand skilled operators and precise control systems, posing challenges for decentralized or smaller treatment plants.
- Environmental Impact: Some technologies, may generate by-products or require significant energy, potentially offsetting their environmental benefits.
To effectively combat antimicrobial resistance in wastewater, combining these technological advances with robust policy measures is crucial. Policies that address financial constraints, promote technology transfer, and enforce regulations can help bridge the gap between innovation and practical application.
Why are policy and regulatory approaches crucial?
While advanced treatment technologies play a huge role in mitigating the effects of AMR in wastewater, it is important to recognize that the primary driver of antibiotic contamination in water systems is overuse and misuse of antibiotics in healthcare and agriculture. Addressing these root causes through strong policy frameworks and regulatory enforcement is essential to reducing the overall burden of AMR.
Current Scenario in India
Drugs and Cosmetics Act (1940): India’s primary law governing the sale, distribution, and use of pharmaceuticals is the Drugs and Cosmetics Act, enacted in 1940. This Act focuses on regulating the import, manufacture, distribution, and sale of drugs and cosmetics to ensure their safety, efficacy, and quality. It establishes guidelines for the licensing, labelling, and distribution of drugs, while also specifying standards for drug manufacturing practices.
To address AMR, the Act includes provisions such as the categorization of certain antibiotics under Schedules H and H1. Schedule H drugs require a prescription for sale, while Schedule H1, introduced in 2013, places stricter controls on the sale of specific antibiotics by mandating the maintenance of detailed records of sales by pharmacies, including the name and address of the prescriber and the patient, for three years. This measure aims to restrict over-the-counter (OTC) sales and curb antibiotic misuse.
Despite this act, the unregulated sale of OTC continues. Compliance remains a significant challenge due to the following reasons:
- Lack of awareness: Public awareness about the dangers of self-medication and antibiotic resistance is still limited.
- Weak enforcement: There are insufficient checks and monitoring mechanisms to ensure that pharmacies and healthcare providers adhere to the laws.
- Regulation in rural areas: In rural and remote areas, regulation and enforcement are even weaker, leading to higher instances of unregulated antibiotic use.
National Action Plan on Antimicrobial Resistance (NAP-AMR): NAP-AMR was introduced by the Ministry of Health and Family Welfare in collaboration with other key stakeholders in 2017, with the aim of tackling the mounting threat of antimicrobial resistance in India. This comprehensive framework aligns with the World Health Organization’s (WHO) Global Action Plan on AMR and sets out a multisectoral approach to combat antibiotic misuse and resistance. The NAP-AMR focuses on several core objectives:
- Improving awareness about AMR and the consequences of antibiotic misuse.
- Strengthening regulations to control the sale and use of antibiotics.
- Improving surveillance systems for antibiotic use and resistance.
- Encouraging research into alternatives to antibiotics.
While the NAP-AMR represents a strategic step forward, its impact has been hindered by challenges in implementation, particularly at the grassroots level. Many healthcare professionals and members of the public remain unaware of the plan’s objectives and the dangers of antibiotic misuse, with antibiotics still being dispensed without prescriptions in numerous regions.
What we can do moving forward?
To effectively combat antimicrobial resistance in wastewater and beyond, it is crucial to address the gaps in existing systems such as ensuring compliance, and fostering a culture of responsible antibiotic use are essential for creating lasting change.
Translating Policy and Frameworks into Action
While regulations like the Drugs and Cosmetics Act (DCA) govern pharmaceutical sales, stricter enforcement mechanisms are needed to ensure adherence at all levels. Policies are often developed nationally but left to state governments for implementation as enforceable acts or resolutions. The DCA, enacted in 1940 and periodically amended, remains central to pharmaceutical regulation. However, with AMR rising, a future amendment could prioritize tighter control over over-the-counter (OTC) antibiotic sales, requiring prescriptions and enhancing compliance for pharmacists and healthcare workers.
The successful execution of NAP-AMR calls for greater collaboration among ministries, including health, pharmaceuticals, and the environment. Ministries must align to transform the framework into enforceable acts, ensuring broad adherence. This includes implementing robust structures for NAP-AMR, national surveillance systems for antibiotic use, and dedicated resources for state and local authorities. Additionally, leveraging technology can monitor OTC antibiotic sales. Digital prescription systems could track prescriptions, reducing unauthorized sales and forgeries. Integrating Aadhaar with these systems would help ensure accurate tracking and identify misuse patterns, enhancing accountability.
The AYUSH (Ayurveda, Unani, Siddha, Homeopathy) regulations under the DCA, promoting traditional medicine, also play a key role in India’s healthcare. Aligning these practices with the AMR agenda, regulating antibiotic use in traditional medicine, and involving AYUSH practitioners in AMR awareness can strengthen the fight against AMR. Expanding outreach to healthcare providers, improving stewardship, and fostering collaboration with pharmacies, community leaders, and educational institutions will support compliance and drive meaningful change.
Public Awareness Campaigns
The major barrier to addressing AMR is a lack of awareness among the public, healthcare communities, and farmers. Addressing this requires robust education and outreach efforts. A foundational approach involves a national-level Behaviour Change Communication (BCC) campaign led by the government, similar to successful initiatives for polio eradication and tuberculosis awareness. Such a campaign can educate the public about antibiotic misuse through mass media, community programs, and interactive initiatives. Building on public awareness, it is crucial to educate farmers on the responsible use of antibiotics in animal husbandry to reduce AMR risks at the source. By equipping farmers with knowledge of prudent antibiotic use, we can limit the spread of resistant bacteria more effectively than focusing solely on technical waste management practices.
To ensure long-term change, incorporating AMR awareness into school curriculums provides an opportunity to educate children and young people early. Instilling an understanding of antibiotic stewardship from a young age helps foster a culture of responsible antibiotic use and builds future generations of informed citizens.
Reinforcing these efforts, placing informative posters and materials at pharmacies can serve as timely reminders about proper antibiotic use and the dangers of resistance, reaching individuals at critical moments of sale and use. This strengthens public awareness campaigns by directly engaging with consumers at points of care. Finally, healthcare providers are pivotal in mitigating AMR. Continued education and training programs could be suggested to promote antibiotic stewardship, reduce over-prescription, and encourage adherence to best practices in patient care. These measures, taken collectively, can build a foundation of awareness and responsible behaviours that are crucial in combating the growing threat of AMR.
Effective Wastewater Management
Combining regulatory measures for antibiotic use with strategies to manage antibiotic residues in wastewater is essential in the fight against AMR. A key step is mandating Zero Liquid Discharge (ZLD) in pharmaceutical industries, where all water used must be recovered and reused, leaving no discharge. The Central Pollution Control Board (CPCB) already requires ZLD for certain “highly polluting” industries, with implementation overseen by State Pollution Control Boards. Tamil Nadu, for example, mandated ZLD for textile processing and tannery industries as part of its Cauvery River conservation plan, a model adopted by states like Gujarat and Maharashtra. Given the growing threat of AMR, ZLD should be mandated for all pharmaceutical industries to prevent antibiotic contamination in water bodies, with strict monitoring to ensure compliance.
In addition, wastewater treatment facilities must adopt advanced technologies to remove antibiotic residues effectively. Financial incentives can drive the adoption of these technologies, ensuring safer water discharge and reducing environmental contamination.
Agriculture is another significant contributor to AMR, with wastewater and antibiotic-laden manure entering the environment. Farmers must be trained on safe wastewater disposal and responsible manure management. By promoting sustainable wastewater and manure management practices, the agricultural sector can help mitigate AMR risks.
Together, ZLD policies, advanced wastewater treatment technologies, and responsible agricultural waste management can reduce the spread of AMR, protecting both public health and the environment.
Conclusion
Antimicrobial resistance is a complex and growing threat that requires a comprehensive and multifaceted response. While advanced treatment technologies are crucial for mitigating AMR in wastewater, the core issue stems from the overuse and misuse of antibiotics in both healthcare and agriculture. By integrating technological advancements with robust policy measures and creating public awareness, we can take significant steps toward combating AMR.
Author: Lakshmi Priya BS